Introduction
Erythema nodosum is the most common form of septal panniculitis, typically presenting as painful, erythematous nodules on the bilateral anterior shins.1 It is associated with a broad spectrum of etiologies, including infections, autoimmune conditions, medications, and often idiopathic origins.2 The pathophysiology is believed to involve a delayed type IV hypersensitivity reaction.2 Erythema nodosum is more common in women, particularly between the second and fourth decades of life.3,4 Although the association between oral contraceptive pills and erythema nodosum has been documented,5,6 most reports have focused on combined estrogen-progestin formulations.7 This case highlights the development of an atypical presentation of erythema nodosum following the initiation of a progesterone-only oral contraceptive pill, drospirenone, underscoring the need for awareness of hormonal triggers, even with progestin-only agents.
Case Presentation
A 33-year-old female presented to the Internal Medicine clinic with a three-week history of progressive bilateral lower extremity swelling and painful nodules on her shins with overlying desquamation of the skin, predominantly affecting the left side. She reported difficulty ambulating due to severe pain and had transitioned to using a scooter. Notably, symptoms began two days after initiating drospirenone, a progesterone-only oral contraceptive pill prescribed for prior oral contraceptive-induced arthralgias.
Initial evaluation in the emergency department noted bilateral lower leg swelling with erythematous, tender nodules, leading to empirical treatment with cephalexin for presumed cellulitis. Symptoms worsened, and the patient returned to the emergency department three days later with nodules on her right elbow and worsening shin involvement. Chest radiography was unremarkable, and a clinical diagnosis of erythema nodosum was made. She was prescribed a seven-day course of prednisone and opioids for pain control. Although symptoms improved transiently, they recurred promptly after completing the steroid course. Doxycycline prescribed at an outside clinic also failed to provide relief.
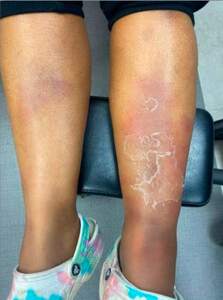
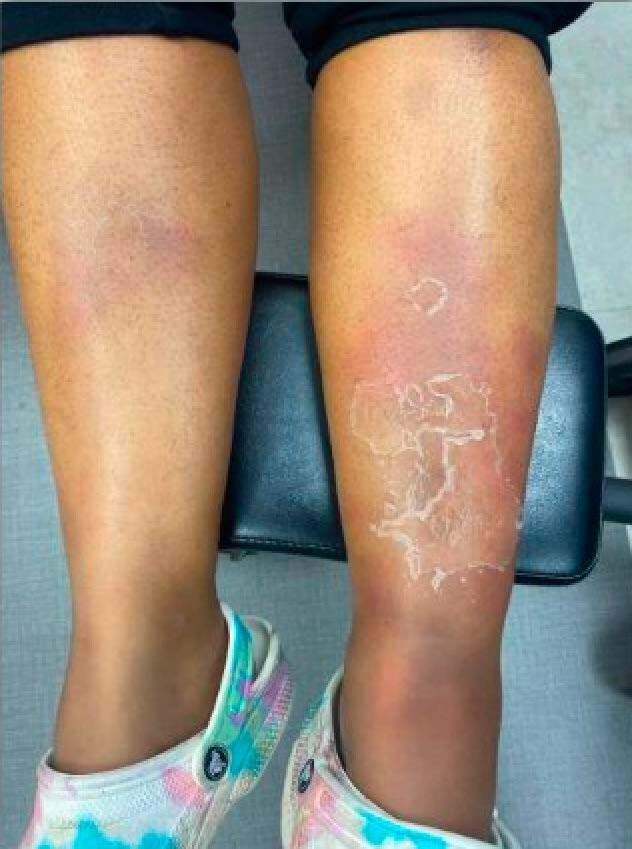
In the Internal Medicine clinic, she presented with persistent painful nodules and edema. She had stopped taking drospirenone two weeks prior. Physical examination revealed firm, tender nodules on bilateral shins, with overlying desquamation and pitting edema on the left leg as seen in Clinical Image 1. Doppler ultrasound ruled out deep vein thrombosis. Laboratory tests showed leukocytosis, a positive anti-nuclear antibody, elevated erythrocyte sedimentation rate, negative vasculitis panel, and normal thyroid function. She was referred to Dermatology and Rheumatology for further evaluation.
Dermatologic examination confirmed suspicion of erythema nodosum, though noted the presentation was atypical due to extensive edema and confluent erythema. Punch biopsy from the right shin revealed thickened fibrous septae with acute and chronic inflammation in the subcutis, most consistent with erythema nodosum. Rheumatologic workup was negative for autoimmune pathology. The patient was treated with non-steroidal anti-inflammatory medications for pain and monitored closely.
At seven-week follow-up in Internal Medicine clinic, the patient had complete resolution of symptoms, with only mild residual discoloration. She had returned to full mobility and daily activities. The multidisciplinary team concluded the likely etiology was erythema nodosum secondary to drospirenone.
Discussion
This case emphasizes the importance of considering hormonal medications—specifically progesterone-only contraceptives—as potential triggers for erythema nodosum. While erythema nodosum is classically self-limiting, its impact on mobility, quality of life, and diagnostic complexity can be profound. Many patients report additional symptoms with erythema nodosum including weight loss, malaise, low-grade fever, and arthralgias.2 This patient experienced significant physical and emotional distress, unnecessary antibiotic courses, and multiple healthcare encounters before a unifying diagnosis was made.
Notably, the presentation was atypical with pitting edema and overlying desquamation, which are less common features of erythema nodosum. The recurrence of symptoms following steroid taper and non-response to antibiotics further highlighted the need for a high index of suspicion and appropriate biopsy in unclear cases. Biopsy of erythema nodosum classically exhibits inflammatory infiltrate in the septa between subcutaneous fat lobules with the presence of Miescher’s radial granulomas and the absence of vasculitis.1,2 Biopsy of late lesions may also show fibrous thickened septa with inflammatory cells.8
Although erythema nodosum often resolves within two-to-eight weeks without scarring, early identification of the underlying trigger is crucial to minimizing morbidity.3 In patients presenting with nodular eruptions and a recent history of medication changes, particularly hormonal agents, erythema nodosum should be included in the differential diagnosis.
When treating drug-induced erythema nodosum, discontinuing the inciting medication is highly recommended. Other therapeutic measures include supportive care such as compression bandages and limb elevation to reduce edema and pain.9 Non-steroidal anti-inflammatory medications can be useful to mitigate pain.10,11 In cases of refractory erythema nodosum, colchicine and potassium iodine have been shown to provide benefit.8,12 Systemic corticosteroids are rarely used to treat erythema nodosum but may be considered in severe cases.13 Ruling out infection is of utmost importance prior to starting corticosteroids in patients with erythema nodosum especially given erythema nodosum is commonly caused by numerous infections.13
Erythema nodosum has historically been documented resulting from combination oral contraceptives with initial speculation for estrogen being the contributing hormone.7 More case reports like this one are supporting erythema nodosum as a side effect of progesterone-only oral contraceptives as well.
Importantly, this case contributes to the growing recognition of progesterone-only oral contraceptives as potential triggers for erythema nodosum and suggests that clinicians should monitor for hypersensitivity reactions even in the absence of estrogen. Literature suggests that switching to a different progestin formulation may not always cause recurrence, but further research is needed.
Conclusion
This case underscores the need for clinicians to consider erythema nodosum in patients with painful nodules and recent oral contraceptive changes, even with progesterone-only formulations. Timely recognition and management can significantly improve patient outcomes and reduce unnecessary treatments and healthcare visits.
Informed Consent
The patient in this case gave informed consent verbally on September 16, 2025, for this manuscript.